This can only be fully performed after the patient has woken and by asked about symptoms however, as this may not be for a significant period of time, conclusive radiological investigations are sought to rule out injury. Therefore, spinal immobilization is continued until injury can be ruled out and the spinal column ‘cleared’. However, in the unconscious patient, no pain or tenderness may be reported, and the clinician may have no idea about neurological signs and symptoms (unless these were recorded before the coma ensued). In the awake patient, diagnosis of spinal injury is greatly aided by the ability of the patient to report pain, comply with instructions, and allow detailed clinical examination. In the vast majority, no spinal column injury will eventually be identified. Patients who are fully immobilized after trauma are commonplace in Emergency Departments. In other words, the patient is assumed to have a neck injury until proven otherwise, and is transported to hospital and managed as such. Properly applied, this requires both a rigid collar and a spinal board with sandbags and tape, to keep the head completely still and the spinal column ‘in-line’. 2 The standard pre-hospital practice for any patient who has suffered injury or trauma (often this may only have been relatively minor) is to have full spinal immobilization at the scene of the incident. The appreciation of the increased risk of cervical spine injury in trauma victims with neurological impairment prompted the development of ATLS guidelines for the management of trauma patients. Factors making injury more likely include focal neurological deficit, concurrent head injury, and a Glasgow Coma Scale (GCS) of <8. 1Ĭervical spine injury has an incidence of 5% in association with blunt polytrauma. In England in 2004–5, cervical spinal cord injury was recorded in 637 cases. The financial cost for tetraplegic individuals may run into millions of pounds for lifetime medical care. Cervical spinal cord injury is a devastating event both for both the patient and society.

The most common aetiologies are road traffic accidents, falls, assaults, and sporting injuries. EpidemiologyĬervical spine trauma occurs most frequently in males between the ages of 20 and 30 yr. It includes a summary of the epidemiology of cervical spine injury, a critique of the relevant guidelines, and a discussion of more recent evidence, which may be used to guide clinical practice. When CT scanning and radiography detect no fractures or signs of instability, MR imaging does not help in determining cervical stability and may lead to unnecessary testing when not otherwise indicated.This article describes the issues concerning the common problem of safely excluding potentially unstable cervical spine injury in patients who cannot be assessed clinically because of their depressed level of consciousness. Magnetic resonance imaging is sensitive to soft-tissue injuries of the cervical spine. Six of the latter underwent dynamic testing, which demonstrated normal results.Ĭonclusions. Furthermore, there were 143 patients with abnormal CT or radiographic study findings, in 13 of whom MR imaging revealed normal findings. In each case of cervical instability (65 patients) CT, radiographic, and MR imaging studies demonstrated abnormalities. Of these 70 patients, 23 underwent dynamic imaging, the findings of which were normal. Of 166 patients in whom CT scanning or radiography demonstrated normal findings, 70 had undergone MR imaging that revealed abnormal findings. Of 6328 patients admitted through the trauma service, 314 underwent MR imaging of the cervical spine. Abnormal soft-tissue (prevertebral or paraspinal) findings on MR imaging were correlated with those revealed on computerized tomography (CT) scanning and plain and dynamic radiography to determine the presence/absence of cervical instability. The reasons for MR imaging screening were neurological deficit, fracture, neck pain, and indeterminate clinical examination (for example, coma). Data in all patients admitted through the Level I trauma service at the authors' institution who had undergone cervical MR imaging were retrospectively reviewed. The goal of this study was to determine whether cervical abnormalities demonstrated on magnetic resonance (MR) imaging are predictive of spinal instability.
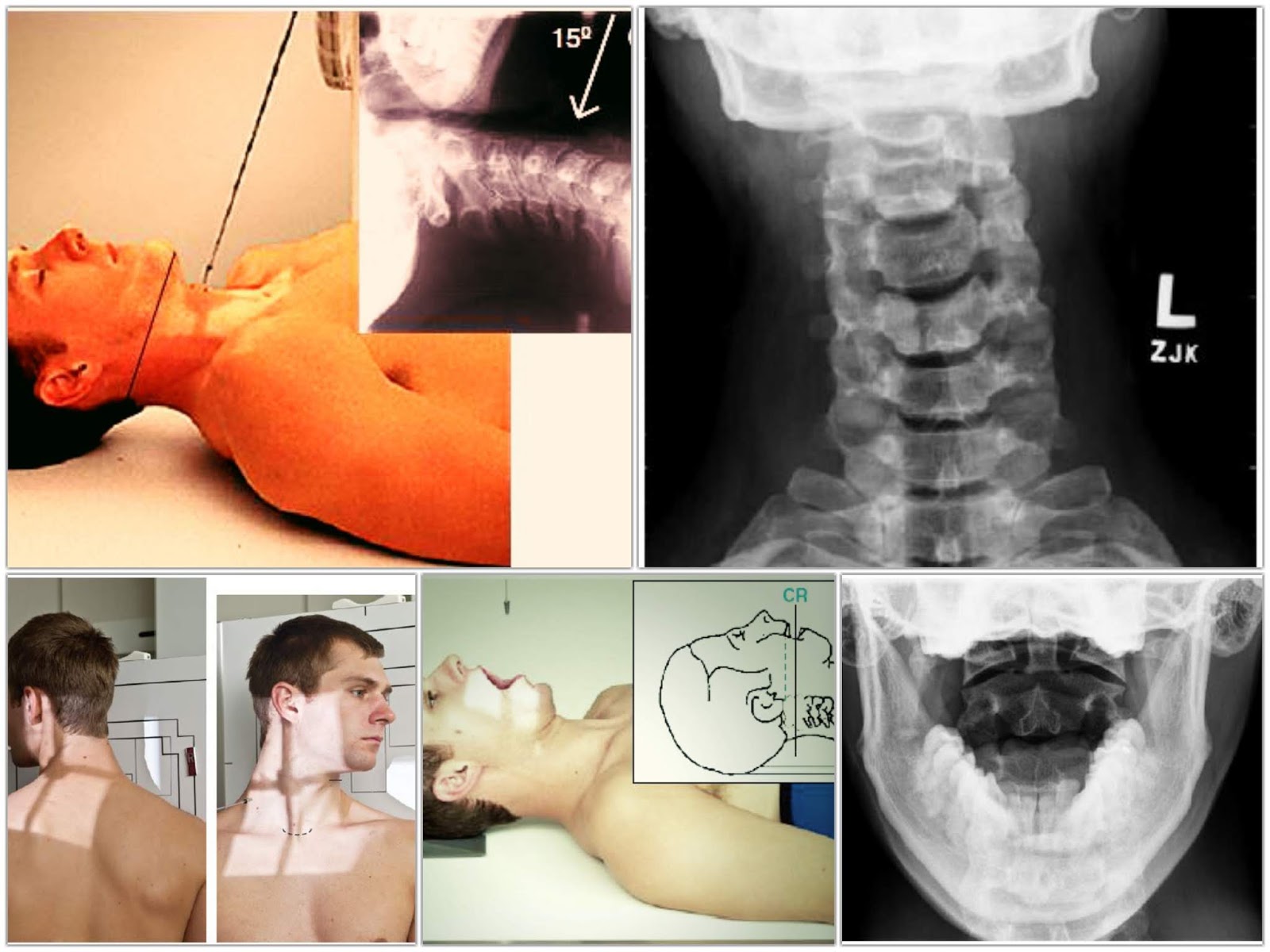
Identifying instability of the cervical spine can be difficult in traumatically injured patients.
